Built to Enhance
Driven by purpose and mission, Nemours continuously invests in models that advance caregiver skills, knowledge and confidence to positively impact children’s health.
Parents, educators and health professionals all have important roles to play in assuring children have the best chance to grow up healthy. From its inception, the Nemours Children’s Health System has designed programs and tools that share best practices, policies and the latest information to support decisions related to children’s health — at home, in the classroom, in the clinic, and in local, state and federal government.
WELL-ROUNDED MDs
Nemours welcomed its first class of pediatric residents in July 2019. The flagship residency program at Nemours Children’s Hospital (NCH) is part of Nemours’ movement to enhance pediatric medical education and practice.
The NCH residency began with robust skills-based and communications-based simulation training and includes continued in-depth simulation opportunities throughout the residency.
Each day, residents participate in a conference or didactic curriculum that provides insight into specialized training or community-facing medical and social advocacy. In addition, residents are expected to interface in daily huddles and on a variety of hospital committees, including quality, med safety and ethics. Residents will also select a research focus as well as engage in community outreach activities.
Recognizing the connections between self-care and patient outcomes, every resident and member of the medical staff, including department chairs, receives a mandatory review with a psychologist for baseline evaluation. A 24/7 crisis hotline and access to immediate therapy sessions provide on-demand intervention to support mental health.
Residency is typically viewed as hospital-based learning. However, Nemours recognizes that when community members lack access to health care, we have to bring health care to them. Being able to interact with the community during my residency is incredibly pivotal to my learning, and also reminds me why I do what I do.
— Emily DiLillo, MD, resident, Nemours Children’s Hospital’s inaugural pediatric residency class
Providers Eager to Improve Social Determinants
A recent symposium for Nemours physicians and associates offered a day-long immersion in education about social determinants of health (SDOH). “Attacking the 70%: Understanding the SDOH” included presentations on disparities in the justice system, the role of medical-legal partnerships and the significant role of social workers, along with information on Nemours’ current programs, resources and efforts to promote value and address SDOH.
Fantastic conference! Appreciate the opportunity to discuss and learn.
Symposium attendees also participated in “The Cost of Poverty Experience,” an interactive simulation that portrayed real stories of families impacted by poverty. The experience gave participants insights into factors that patient families may deal with outside of their medical needs.
Simulation Builds Confidence for Parents and Providers
Nemours Institute for Clinical Excellence (NICE) is on the leading edge of pediatric simulation. For the NICE team in Delaware, that includes pediatric patient- and family-centered simulation that is both nationally and internationally recognized.
Nemours/Alfred I. duPont Hospital for Children (N/AIDHC) is in its 10th year of delivering eight different simulation-based courses that attract multidisciplinary participants from across the U.S. In 2019, N/AIDHC was only the fourth site in the U.S. to host the international Trauma Resuscitation for Kids course in conjunction with the Royal College of Physicians and Surgeons of Canada and the U.S.-based Pediatric Trauma Society.
Since 2016, Nemours has required simulation training for caregivers of children who receive a tracheostomy before they are discharged home. In an effort to keep skills from declining, plans are in the works to offer quarterly refresher courses for families at N/AIDHC. In Central Florida, the NICE team is also developing after-hours sessions at Nemours Children’s Hospital through a donor-supported initiative called Simulation Enhanced Learning for Families (S.E.L.F.) Care.
In addition to improving the quality and safety of patient care, NICE teams use simulation to improve systems integration. Across Nemours, that includes “day-in-the-life” simulations to identify latent safety threats or hiccups in processes, allowing for changes before opening a new facility. Several new Nemours locations participated in these simulations in 2019 — Nemours Sports Medicine at the 76ers Fieldhouse, the Advanced Delivery Unit at N/AIDHC and the Nemours Cardiac Center, Florida.
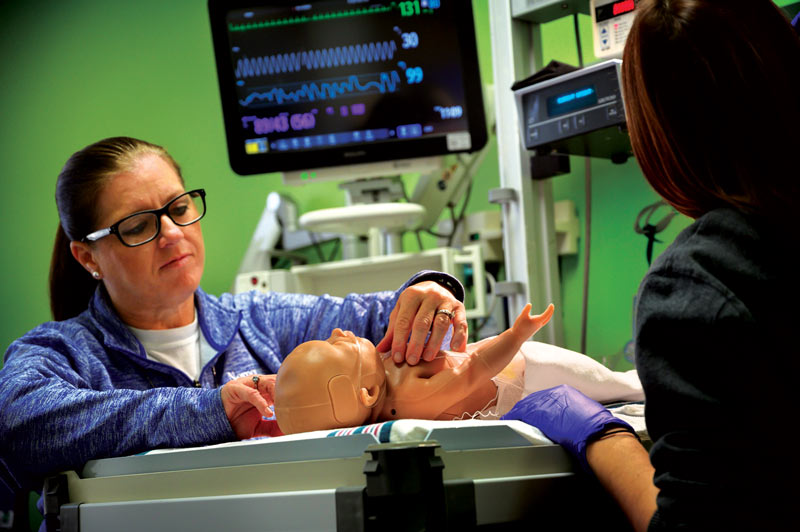
The NICE Sim Lab team is vitally important to the quality of care we deliver. We could say confidently that the new operating room was ready for patients.
– Pete Wearden, MD, PhD, Director, Nemours Cardiac Center – Florida
Tools to guide and teach with empathy
Children who exhibit disruptive behaviors in the classroom may have more going on than meets the eye. Root causes like speech or language delays or trauma in the home may be contributing factors. If left unattended, these factors can have a deleterious impact on a child’s health and their long-term quality of life. New programs developed by Nemours Florida Prevention Initiative are designed to help early childcare educators learn how to identify at-risk children and work with their parents to manage behaviors.
With funding support from the Winter Park Health Foundation, Nemours developed GATEway (Guiding and Teaching with Empathy), a program designed to build a strong alliance between parents/caregivers and childcare educators. The multipronged approach aims to improve the emotional, behavioral and mental health of children by teaching them skills and techniques to self-regulate and improve resiliency. These are reinforced by guiding positive parenting strategies and self-efficacy to help the child at home, including access to telehealth consultations when parents may be struggling in the moment.
A pilot, launching in 2020, includes a cohort of four early care and education centers with children as young as infants through age five.

Healthy Kids, Healthy Future
Healthy Kids, Healthy Future Technical Assistance Program (HKHF TAP) is funded by a five-year CDC Cooperative Agreement. This program provides high-quality technical assistance (TA) and supports 12 state partners’ efforts to integrate healthy eating and physical activity best practices into Early Care and Education (ECE) systems and settings.
The HKHF TAP program advocates best practices such as ensuring toddlers and preschoolers receive fruits or vegetables at every meal and that infants have short periods of “tummy time” every day.
Using the CDC’s Spectrum of Opportunities framework, Nemours collaborates with departments of health, child care resource and referral agencies, and other ECE organizations to accelerate the integration of best practices into broader state systems, such as TA networks, professional development, licensing, Child and Adult Care Food Program, and Quality Rating and Improvement Systems.
Learn more about Healthy Kids, Healthy Futures at HealthyKidsHealthyFutures.org.

Prior work by Nemours with the National Early Care and Education Learning Collaboratives project funded by the CDC helped nearly 1,200 child care programs in 10 states improve their healthy eating and physical activity standards. Learn more here.
The Ever-Evolving Provider Skillset
From medical students and residents to physician fellows, senior physician leaders and all stages in between, Nemours provides opportunities to build, enhance and refresh the skills necessary to support the future of health delivery.
- using pediatric simulation to develop clinical proficiency and communication skills
- creating pipelines to ensure inclusivity and building understanding toward health equity
- encouraging curiosity and providing access to innovative technologies, unparalleled data and research mentors
- emphasizing wellness and self-care, including access to dedicated mental health resources